COVID-19 infections, hospitalizations and deaths have been steadily climbing in Texas since December. The latest data from the Texas Department of State Health Services (DSHS) show there were more than 19,000 new COVID-19 cases for the week of Jan. 7.
DSHS also reported a 30.4% increase in COVID-19 related deaths that week in comparison to weeks prior.
Jeffrey SoRelle, an assistant professor of pathology with UT Southwestern Medical Center, has been tracking COVID-19 variants since the pandemic began.
He said a newer variant of omicron, called JN.1, has been “driving a lot of the increase in cases.”
“This variant has actually been around since September but hasn’t really taken off until the last few months,” SoRelle said.
In October, the U.S. Centers for Disease Control and Prevention reported that JN.1 made up about .1% of all COVID-19 cases in the country. Now, it makes up almost 85%.
SoRelle said the winter holidays and increased travel may have given the virus “the right conditions to become more infectious and find more people to jump into.”
JN.1 seems to be more infectious than previous variants. Researchers from the University of Tokyo in Japan wrote it could be “one of the most immune-evading variants to date,” and a December report from the World Health Organization said JN.1 had “higher immune evasion properties” compared to other omicron variants.
One way researchers measure how the virus changes over time is by looking at the spike protein, which is part of how viruses bind to cells in the body and replicate. COVID-19 variants have mutations in the spike protein, which is how SoRelle tracks how it can “evade immunity and lead to changes in infectiousness.”
He said JN.1 has more than 30 mutations in the spike protein.
“When we see that many, that’s a very large difference that came out of nowhere, pretty much,” SoRelle said.
But there isn’t evidence so far that JN.1 is causing more severe illness. SoRelle said there are some studies that have explored how the new variant is “impacting different kind of lung cells than it has before,” but doctors haven’t seen that in patient cases yet.
SoRelle said it’s the difference between an upper respiratory infection—which is common with RSV, the common cold, and the flu—versus a lower respiratory infection in the lungs.
“An upper respiratory infection is, you’re coughing, or you have a runny nose, [or] sore throat,” he said. “When things start infecting the lower lungs, they prevent the air sacs from filling. Then they get filled with fluid or become inflamed and that really prevents you from breathing. That’s where people get into trouble with worse symptoms that can be more life-threatening.”
The best way to prevent COVID-19 infections now, said SoRelle, is to stay up-to-date on vaccinations.
An updated COVID-19 shot came out in the fall, but uptake’s been slow—only about 21% of adults nationally, and about 17% of Texans, have gotten the new vaccine, according to the CDC.
“Most people have now either been exposed and infected, or vaccinated, and sometimes both,” SoRelle said. “We have a lot of built-up immunity, but there are extra tools that we have to help protect us.”
And during the peak of respiratory virus season, which falls between December and February, SoRelle encourages people to stay home if they’re exhibiting symptoms, use at-home tests, and consider wear a mask in crowded or indoor spaces to prevent virus spread.
Copyright 2024 KERA. To see more, visit KERA.


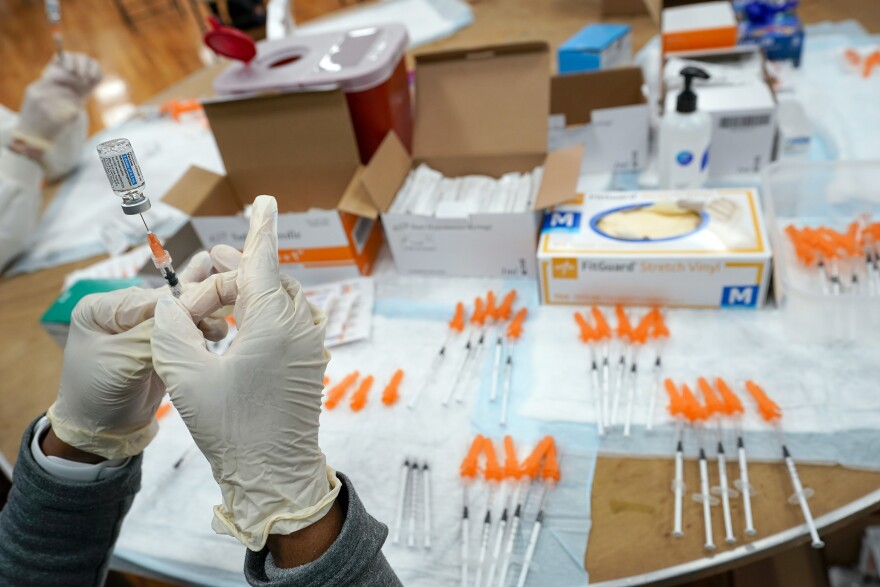
!["Even though [COVID-19] pales in comparison to last year, we don't know where this is going to trend," said Juan Rodriguez, chief epidemiologist for Denton County Public Health. (AP Photo/Seth Wenig)](https://npr.brightspotcdn.com/dims4/default/659aefa/2147483647/strip/true/crop/6000x4000+0+0/resize/880x587!/quality/90/?url=https%3A%2F%2Fnpr.brightspotcdn.com%2F23%2F39%2F21094a9b4e76ba09fcf4f437dfeb%2Fap23004761194102.jpg)